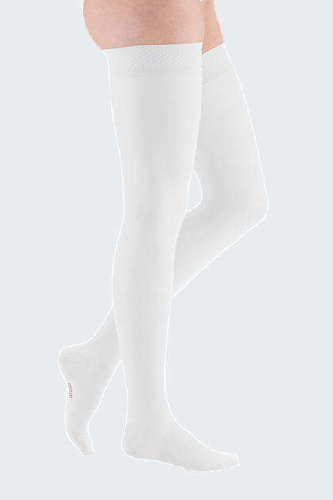
Venous insufficiency and pulmonary embolisms - what’s the difference?

Venous insufficiency and pulmonary embolisms both affect the legs of non ambulatory and ambulatory patients - however, how these conditions are treated and prevented differ significantly.
Venous insufficiency and pulmonary embolisms - what’s the difference?
You may have heard mention of at least one of these conditions, especially if you suffer from artery and vein complications. Although these conditions affect the blood vessels, they are distinctly different from one another. So, what exactly are embolisms and venous insufficiency, how do they affect the human body, what are their symptoms and how exactly do you treat these conditions? Let’s dive right in and find out!
Venous insufficiency is the condition that impedes on blood circulation from your limbs back to the heart, causing the blood to oftentimes pool in the veins of your legs, which can lead to varicose veins (Healthline). Varicose veins are enlarged and improperly functioning veins that have a distinct enlarged bulging look to them. Venous insufficiency is most often caused by previous cases of a blood clot (deep vein thrombosis) and varicose veins, however, other risk factors include obesity, smoking, cancer, muscle weakness, leg injuries, remaining immobilie for long periods of time, and even a family history of venous insufficiency (Healthline). So, how do you know if you have venous insufficiency? There are a number of symptoms you ought to look for, including swollen, itchy and weak legs, leg cramps, ulcers, tight calves, heaviness of the legs and possible skin discoloration (Healthline).
Although you’re likely to notice the symptoms of this condition, it is recommended that you get a full diagnosis from a certified medical specialist, who will more than likely begin the assessment with a physical examination. Upon doing so, they will do a venogram test and a duplex ultrasound (Healthline). The venogram test involves getting intravenous contrast dye being put into your veins, in order to give the doctor a better view of your blood vessels on the X-ray. The duplex ultrasound on the other hand is used to to view the speed and direction of your blood flow, in order to spot any abnormalities (Healthline).
Embolisms, on the other hand, are when an embolus (a particle found in the bloodstream) gets too large and ends up being lodged in a blood vessel, starving the cells of oxygen, leading to their deaths (MediResource). Although there are a number of different embolisms, including brain, retinal, septic, amniotic, air and fat embolisms, we’re going to focus on the pulmonary, as it is usually formed in the legs (MediResource). Pulmonary embolisms (also known as deep vein thrombosis) are formed in the legs and tend to get lodged in the arteries of the lungs, which can prove to be fatal (MediResource). The most common risk factors for this condition are smoking and heart disease, as well as high blood pressure, atherosclerosis, high levels of cholesterol and obesity (MediResource). Unlike Venous insufficiency, pulmonary embolisms don’t come with visible symptoms. You might have this condition if you experience coughing, shortness of breath, back and chest pain and bloody sputum (MediResource). The most accurate way to assess whether or not you have this condition is by taking an X-ray or a ventilation perfusion scan, as well as a doppler ultrasound of the legs in order to spot any blocked arteries (MediResource).
Treatment options
Although both of these conditions affect the legs, it is important to note that they require different treatment options. When it comes to treating venous insufficiency, treatment options vary, depending on your current health, as well as symptoms, age and the severity of your condition (Healthline). You may be recommended a number of treatment options, including:
- Improving blood flow - this can be done with the help of regular exercise, wearing compression stockings and keeping your legs elevated when possible (Healthline).
- Taking medications - most importantly, anticoagulants, as well as those that help improve blood flow (Healthline).
- Surgery - more serious cases of this condition may require surgery, such as vein bypass, surgical vein repair or removal and possibly laser surgery.
However, one of the most common treatment options are graduated compression stockings. These professional grade medical products are made of durable, high-quality materials that apply pressure to the legs, helping to improve blood circulation and prevent blood from pooling in the legs. Compression stockings each have their own compression level, which are subdivided into grade classes, depending on how much pressure is required for treating the individual’s condition. These stockings function by providing compression at the ankles and gradually reducing it towards the thighs. They are lightweight and discrete, making them easy to wear for nearly every occasion.
When it comes to treating ambulatory patients who are suffering from an embolism, doctors usually recommend anticoagulants (which prevent blood clots), leading a healthier lifestyle (without smoking, poor diet and lack of exercise) and utilising anti-embolism stockings. These stockings are widely used by ambulatory and non ambulatory patients alike in order to reduce the risk of DVT, but also to expedite the healing process after vein surgery. The anti embolism variant provides graduated compression to the legs, however, it isn’t recommended to people who have vascular disease affecting their legs (Surgical Directorate). These products are made of comfortable and elastic materials that are durable and fit the wearer with ease.
So, what is the difference between anti embolism and compression stockings? Although both stocking types are worn on the legs, they are applied for different reasons. Anti embolism legwear is worn in order to prevent blood from pooling in the legs, which can occur if you’re immobile due to illness - leading to an increased risk of blood clots (MediResource). Also, they’re not recommended to people who either suffer from poor blood circulation in the lower legs and feet (MediResource). Compression stockings on the other hand are recommended to people who are already in the early and or advanced stages of venous insufficiency and are showing signs of spider veins and varicose veins.
Whether you’re suffering from varicose insufficiency or are looking to prevent embolisms, it is essential that you consult with your doctor prior to purchasing stockings, as they are medical products and aren’t a “one-size-fits-all” solution. Once you’ve consulted with a medical specialist and know which compression level stockings are needed, you’re ready to go shopping. Visit our store to find reliable anti-embolism stockings that will help you prevent deep vein thrombosis and blot clots, as well as compression stockings to help treat spider and varicose veins.
Sources:
- “Venous insufficiency” Healthline Editorial team, September 27th, 2018 https://www.healthline.com/health/venous-insufficiency
- “Embolism”, MediResource Clinical Team https://www.medbroadcast.com/condition/getcondition/embolism?_ga=2.66075753.633801179.1605912879-355012069.1605912879
- “Anti-embolism stockings your questions answered”, Surgical Directorate January 2015 https://www.ouh.nhs.uk/patient-guide/leaflets/files/11368Pstockings.pdf
Recommended
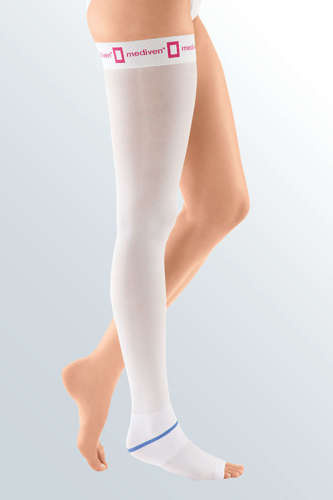
Anti-embolism thigh length compression stocking with silicone topband (1 piece) mediven struva 35 medi

mediven struva 23 anti-embolism thigh length stockings with waist attachment